Lipoatrophy الضمور الشحمي
HTML clipboard
INSTRUCTION
Look at this patient
Look here (the examiner pointing at the patient's thighs).
SALIENT FEATURES
History
-
Whether the patient is taking insulin for diabetes.
-
Past history of renal disease (mesangiocapillary glomerulonephritis).
-
History of HIV and whether patient is receiving antiretroviral agents.
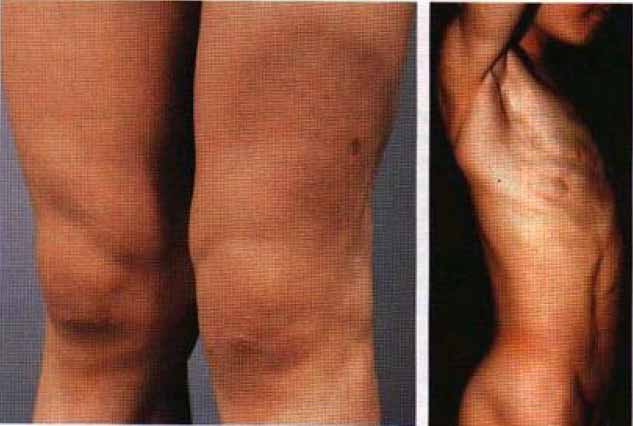
Examination
Atrophy of the subcutaneous fat leading to disfiguring excavations and depressed areas.
DIAGNOSIS
This patient has atrophy of subcutaneous fat or lipoatrophy (lesion) due to local injectionof subcutaneous insulin (aetiology).
ADVANCED-LEVEL QUESTIONS
With which conditions is lipoatrophy associated ?
-
Mesangiocapillary glomerulonephritis.
-
Localized scleroderma.
-
Morphoea.
-
Chronic relapsing panniculitis.
-
HIV.
What advice would you give this patient on insulin ?
The insulin should be changed to a more purified form. The purified form should beinjected directly into the atrophic area, which often results in the restoration of the localcontours.
What is the mechanism of lipoatrophy atrophy ?
This complication results from an immune reaction
Can lipohypertrophy occur with insulin injections ?
Yes, as a consequence of the pharmacological ettects ot lnsuhn being repeatedlydeposited in the same location. Rotation of injection sites can prevent this com-plication.It can occur with purified insulins and responds best to liposuction.
What is the relationship between lipoatrophy and HIV ?
Patients infected with HIV-I receiving antiretroviral therapy have been reported to haveabnormal fat distribution including (a) lipoatrophy or loss of subcutaneous fat, and (b)central or visceral fat accumulation.
Typically these patients have wasting of face andlimbs along with adipose tissue accumulations in the abdomen and back of the neck,the latter giving a 'buffalo hump' appearance.
It was initially considered to be causedonly by HIV-1 protease inhibitors but subsequently has been found in patients who havenever received these agents and, moreover, there is no reversion of the lipodystrophyfollowing withdrawal of protease inhibitors. More recently, lipoatrophy has beenassociated with nucleoside reverse transcriptase inhibitors (NRTIs) and is said to bedue to interference with lipid metabolism and the mito-chondrial toxicity of these agents(Lancet 2001; 357: 592-8).The 1923 Nobel Prize in Medicine was awarded for the discovery of insulin to aCanadian surgeon, Sir Fredrick G. Banting (1891-1941) and Scottish physiologist, JohnJ.R. Macleod (1876-1935) working in Toronto. Banting shared his monetary prize withCharles Best whereas Macleod shared his prize with J.J. Collip (the latter purified insulinto the point that it could be used in humans). Macleod corrected Banting's deficiencieson carbohydrate metabolism and provided him with laboratory support including theservices of a graduate student in physiology, viz. Charles Best. Macleod was fromAberdeen.
