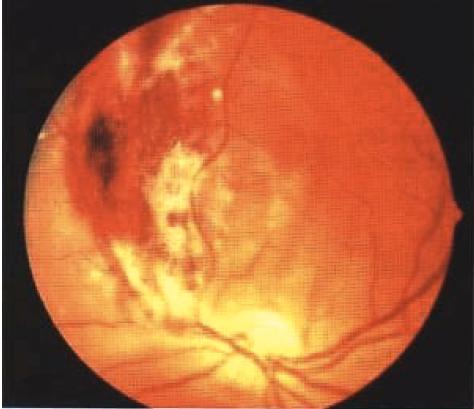
Retinal changes in AIDS التغيرات الشبكية في مرض الايدز - عوز المناعة المكتسب
INSTRUCTION At a distance from the patient, the examiner will say that this patient has HIV, examine his fundus. SALIENT FEATURES History · Floaters. · Red eye. · Impaired vision. Examination Patient 1: Cottonwool spots Cottonwool spots (Fig. 86). Proceed as follows: Tell the examiner that you would like to exclude diabetes and retinal vascular disease. Patient 2: Cytomegalovtrus (CMV) retinitis. · An area of retinitis with nerve fibre layer infarcts, haemorrhages, retinal opacifi-cation and perivascular sheathing - 'pizza-pie fundus'. · Tell the examiner that you would like to do a CD4 count (<50 in acute infection). QUESTIONS How would you treat cottonwool spots? In a patient with known HIV infection, such infarcts require no specific therapy. ADVANCED-LEVEL QUESTIONS How would you treat the lesions of CMV retinitis? · Therapy with intravenous ganciclovir or foscarnet is given lifelong to protect unaffected areas but does not restore functional areas already affected. The optimal treatment for patients with AIDS, normal renal function and CMV retinitis is foscarnet plus an antiretroviral nucleoside such as zidovudine. For similar patients with impaired renal function, ganciclovir would be the drug of choice, perhaps with an antiretroviral agent such as didanosine that has few over-lapping side-effects. Late retinal detachment occurs despite therapy in one fifth of these patients. · Sustained release ganciclovir implant in the pars plana of the eye. Oral ganciclovir in conjunction with an implant reduces the incidence of new cytomegalovirus disease and delays the progression of retinitis (N Engl J Med 1999; 340: 1063-70). · Intravitreal injections of ganciclovir or foscarnet. What do you know about ganciclovir? It is a derivative of aciclovir. It can cause bone marrow depression and hence should not be administered simultaneously with zidovudine. What do you know about foscarnet? It is an organic analogue of inorganic pyrophosphate. Its side-effects include renal impairment, electrolyte imbalance and seizures. It can be safely administered with zidovudine. What are the other retinal manifestations in patients with AIDS? · Toxoplasmosis retinochoroiditis - usually nasal to the disc, characterized by extensive whitish infarction and inflammation, with minimal associated intra-retinal haemorrhage (outer retinal involvement may show 'brush-fire' advancement of infection). · Pneumocystis carinii choroiditis - characterized by scattered nodular yellowish-orange lesions deep in the retina, usually throughout the posterior pole. · Acute retinal necrosis syndrome - with severe peripheral retinal infarction and retinal vasculitis. Atrophic retinal holes appear later in these areas. · Progressive outer retinal necrosis syndrome - characterized by diffuse whitish opacification of the retina beneath the retinal vessels and a cherry-red spot in the fovea. It is associated with herpes zoster and the prognosis for visual acuity is dismal. · Ocular presentations of syphilis include anterior and posterior uveitis, retinitis, retinal vasculitis and papillitis. · Acute syphilitic posterior placoid chorioretinitis - large placoid yellowish lesions at the level of the retinal pigment epithelium in the posterior retina with inflam-mation of the vitreous and loss of vision. What diagnostic tests would you perform to detect retinal manifestations of AIDS? · Careful clinical observations. · Serology: CD4 count (usually <50 in untreated cases of CMV retinitis). · Culture. · Retinal biopsy by pars plana vitrectomy. · Fluorescein angiography: helpful in differentiating retinal lesions. · Sequential fundus photographs: for diagnosis and monitoring of lesions. · Testing of ocular fluid by polymerase chain reaction. Mention some ocular non-retinal manifestations of AIDS. · Optic neuropathy. · Kaposi's sarcoma of the conjunctiva. · Orbital lymphoma. · Cranial nerve palsies. · Nystagmus.