Erythema multiforme الحمامى عديدة الأشكال
INSTRUCTION
Perform a general examination.
SALIENT FEATURES
History
-
History of preceding sore throat or cold.
-
Drug history (barbiturates, sulphonamides, phenytoin, penicillins).
-
Blister-like skin rash with intense itching.
-
Mouth ulcers (mucosal involvement suggests Stevens-Johnson syndrome).
Examination
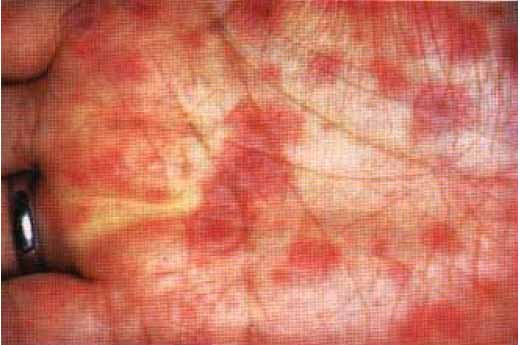
Target-shaped lesions , usually over the limbs. A classical target lesionconsists of three concentric zones of colour change - typically there is a central, dark,purple area or blister surrounded by a pale, oedematous round zone which in turn issurrounded by a peripheral rim of erythema, Pleomorphic eruption with macules, papules and bullae.
Proceed as follows:
-
Look at the mucous membranes of the mouth and eyes (Stevens-Johnsonsyndrome).
-
Tell the examiner that you would like to examine the external genitalia for ulcers.
Note. Erythema multiforme is a cell-mediated hypersensitivity reaction to many differentimmunological insults, including drugs and infectious agents such viruses (most notably herpes simplex). In its so-called 'minor' form, it is manifested byheterogeneous cutaneous eruption, at times bullous.
DIAGNOSIS
This patient has target-shaped lesions (lesion) due to sulphonamides (aetiology) whichusually resolve on discontinuing the drug (functional status).
QUESTIONS
What is the underlying aetiology?
-
Infections (herpes simplex, mycoplasma, streptococci).
-
Drug hypersensitivity (sulphonamides, penicillin, barbiturates, salicylates,antimalarials).
-
Collagen vascular disorder (SLE, dermatomyositis, periarteritis nodosa).
-
Malignancy (carcinomas and lymphomas).
-
Multiple myeloma.· Idiopathic - in 50% of cases no cause may be found.
ADVANCED-LEVEL QUESTIONS
How would you investigate this patient?
-
Viral titres, in particular for herpes simplex type 1.
-
Complement fixation test for mycoplasma.
-
Antistreptolysin O (ASO) titres.If the above are negative:
-
Serum(s) antibodies.
-
Protein electrophoresis, urine for Bence-Jones protein.
What is the histology of erythema multiforme?
-
Early lesions: superficial perivascular lymphocytic infiltrate with oedema of thedermis, accompanied by degeneration and necrosis of keratinocytes and margin-ationof lymphocytes at the dermoepidermal junction.
-
Late lesions: upward migration of lymphocytes into the epidermis; discrete andconfluent portions of the epidermis necrose resulting in blister formation andsubsequently erosions (due to sloughing of the epidermis).
-
Target lesions: characterized by central necrosis surrounded by perivenularinflammation.
What do you understand by the term 'Stevens-Johnson syndrome'?
Stevens-Johnsonsyndrome, also referred to as erythema multiforme major, is characterized by fever andmucous membrane involvement (usually oral cavity, eye and genital) in addition to theeruptions of erythema multiforme.
How would you manage a patient with erythema multiforme and Stevens-Johnson syndrome?
-
Symptomatic treatment with antipyretics, intravenous fluids and antibiotics.
-
Systemic corticosteroids, although the role of steroids is controversial.
-
Other immunosuppressive drugs used in recurrent erythema multiforme andStevens-Johnson syndrome include levamisole, azathioprine, dapsone, thalidomide,high-dose intravenous immunoglobulin and ciclosporin.
-
Aciclovir is recommended by some authors as a therapeutic trial in any patientwith severe recurrent erythema multiforme, even if no preceding herpes simplexinfection has been documented.
-
Other therapeutic options:-Localized care including use of antibiotic creams, ointments, sterile dressings,special beds containing beads, amnion dressings on denuded skin. -Ophthalmologicalcare includes use of artificial tears and topical vitamin A. -Extensive denudation of theskin is best treated in a burns unit.Erythema multiforme is a self-limiting condition, but Stevens-Johnson syndrome may befatal.F.C. Johnson (1894-1934) and A.M. Stevens (1884-1945), both Americanpaediatricians, described this condition in 1922 in a paper entitled A new eruptive feverwith tonsillitis and ophthalmia (Am J Dis Child 1922; 24: 526-33).H. Bence-Jones (1814-1873), English physician, St George's Hospital, London.
