مرحبا بك في هذا المنتدى !
يبدو أنك جديد هنا. إذا كنت تريد أن تتورط، انقر فوق أحد هذه الأزرار!
روابط سريعة
الأقسام
- 9.5K جميع الأقسام
- العلوم الطبية الأساسية Basic Medical Sciences
- علم التشريح العام و الجنين Anatomy and Embryology
- علم وظائف الأعضاء (الفيزيولوجيا) Physiology
- علم النسج Histology
- علم النسج العام ( عدا الأسنان ) General Histology
- علم النسج الخاص بالأسنان Oral histology
- علم الخليةو الحياة Biology
- علم التشريح المرضي Pathology
- التشريح المرضي العام ( عدا الأسنان ) Pathology
- التشريح المرضي الخاص بالأسنان Oral Pathology
- علم الأحياء الدقيقة Microbiology
- الجراثيم و الفيروسات Germs and Viruses
- الطفيليات الطبية Parasitology
- الفطور و الحشرات Insects and Fungi
- علم الوراثة الطبية Medical Genetics
- علم المناعة الطبية Medical Immunology
- 4 العلوم الطبية السريرية Clinical Medical Sciences
- الأمراض الداخلية Internal Medicine
- 4 الجراحة Surgery
- التوليد و الأمراض النسائية Gynacology & Obstetrics
- الصحة الجنسية Sexual Health
- طب الأطفال Pediatrics
- الجلدية Dermatology
- العينية Ophthalamology
- انف و أذن و حنجرة Ear, Nose, and Throat
- الطب المخبري labratory Medicine
- علم الأورام Oncology
- الطب الشرعي Forensic Medicine
- الطب النفسي Psychiatric
- التغذية والطب البديل Nourishments and Alternative Medicine
- طب الطوارئ و الإسعافات الأولية Emergency Medicine And Primary aids
- متلازمات طبية Medical Syndromes
- علم الأشعة Radiology
- طب الأسنان Dental Medicine
- التعويضات المتحركة الكاملة و الجزئية Removable Prothodontics
- المداواة الترميمية operative dentistry
- المداواة اللبية Endodontics
- طب أسنان الأطفال Pediatric Dental
- جراحة الوجه والفكينoral surgery
- التعويضات الثابتة Fixed Prothodontics
- المواد السنية dental materials
- النسج حول السنية periodontology
- التقويم Orthodontics
- منتدى فنيي الأسنان dental technicians
- طب الفم العام general oral medicine
- علم الأشعة Radiology
- حالات سريريةClinical Cases
- أخر مستجدات طب الأسنان last news
- المنتدى الطبي السني العامgeneral dentistry
- علم الصيدلة Pharma
- علم الأدوية
- علم الأدوية Pharmacology
- أدوية الطوارئ Emergency drugs
- المضادات الحيوية Antibiotics
- الأدوبة المسببة للتشوهات الجنينية Teratogenic drugs
- أدوية Drugs
- علم الكيمياء Chemistry
- كيمياء حيوية سريرية Clinical Biochemistry
- الكيمياء العامة و العضوية و الفيزيائية General & organic chemistry & physical
- الكيمياء الحيوية Biochemistry
- الكيمياء التحليلية و التحليل الآلي Analytical chemistry and the automated analysis
- علم عقاقير Pharmacognosy
- الطب البديل Alternative Medicine
- علم الأعشاب الصيدلانية Pharmaceutical Herbs
- التكنولوجيا الصيدلية Pharmatical technology
- الصيدلانيات Pharmaceutics
- الصيدلة الحيوية والحرائك الدوائية Biopharmaceutics & Pharmacokinetics
- الصناعة الدوائية Drug Industry
- علم السموم Toxicology
- الوصفات الطبية Prescriptions
- صيدلية المجتمع و أدوية OTC Medicines OTC
- الكيمياء الصيدلية Pharmaceutical chemistry
- الصيدلة سريرية و صيدلية المشافي Clinical & Hospital Pharmacy
- دمويات و مناعيات hematology & immunology
- مراقبة جودة الأدوية Drug Quality Control
- البيولوجيا الجزيئية Molecular Biology
- الصحة العامة و تلوث البيئة General Health
- المنتدى الصيدلاني العام
- الجودة الغذائية Food quality
- قسم الجودة الطبية Department of Medical Quality
- قسم الجودة العام General Quality Department
- قسم السلامة والصحة المهنية Department of Occupational Safety and Health
- قسم جودة وسلامة الأغذية Department of Food Quality and Safety
- المنتدى الطبي العام
- المنتدى الطبي العام
- منتدى العلوم والتكنولوجيا الطبية Medical Technology
- قانون و أخلاقيات المهنة
- تاريخ و آداب الطب
- الدراسات العليا و الدراسة في الخارج
- امتحانات Medical Exams
- تبادل الكتب الطبية و الميديا و البيانات الطبية
- مواضيع طبية غير مصنفة
- قسم الأسرة و المجتمع
- العناية بالمرأة الحامل و المرضع
- تربية الأطفال
- الصحة العامة
- التغذية الصحية و الغذاء الصحي
- أسريات
- 2 استراحة العيادة السورية
- المنتدى العام
- نشاطات و ترفيه
- 1 إسلاميات
- تطوير الذات و البرمجة اللغوية العصبية NLP
- المنتدى التقني
- مكتبة الصور و التصميم
- 1 المنتدى الثقافي و الأدبي
- المنتدى الرياضي
- منتدى اللغات Foriegn Languages
- الساحة العامة
- ساحة الحوار و النقاش
- ترحيب و تعارف
- قسم الاستشارات الطبية
- البحوث والندوات العلمية
- الاقتراحات و التطويرات
- الأقــســـام الــعـــامــة
- منتدى الحوار العام
- المواضيع العامة القديمة المستردة
- المواضيع الحاوية على مرفقات
علم الدمويات Hematology
Hematology is study of blood and blood disorders
Cells of the body are serviced by 3 fluids
blood
composed of plasma and a variety of cells
transports nutrients, gases and wastes
interstitial fluid
bathes the cells of the body
Lymph
Interstitial fluid that does not directly return to blood vessels.
but first passes thru lymph nodes and then back to blood
Nutrients and oxygen diffuse from the blood into the interstitial fluid & then into the cells
Wastes and carbon dioxide move in the reverse direction
Composition of Blood
Blood is the body’s only fluid tissue
It is composed of liquid plasma and formed elements (Blood cells).
Formed elements include:
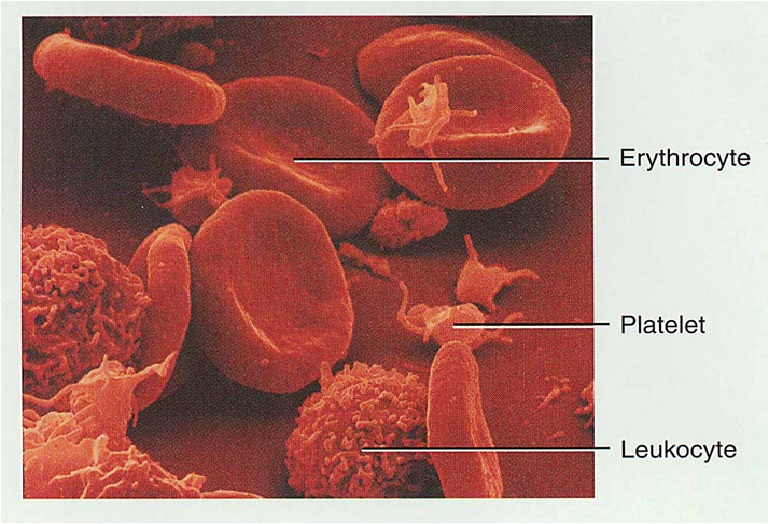
Erythrocytes, or red blood cells (RBCs)
Leukocytes, or white blood cells (WBCs)
Platelets
Hematocrit – the percentage of RBCs out of the total blood volume
Techniques of Blood Sampling
Venipuncture
sample taken from vein with
hypodermic needle & syringe
Why stick an vein?
less pressure
closer to the surface
Finger or heel stick
common technique for diabetics to monitor daily blood sugar
method used for infants
Physical Characteristics and Volume
Blood is a opaque fluid with a metallic taste
Color varies from red to dark red
Temperature is 38C, slightly higher than “normal” body temperature
Blood accounts for approximately 8% of body weight
Physical Characteristics
Thicker (more viscous) than water
Flows (Run)more slowly than water
pH 7.4 (7.35-7.45)
Blood volume
5 to 6 liters in average male
4 to 5 liters in average female
There is hormonal negative feedback systems witch maintain constant blood volume and osmotic pressure
Cells of the body are serviced by 3 fluids
blood
composed of plasma and a variety of cells
transports nutrients, gases and wastes
interstitial fluid
bathes the cells of the body
Lymph
Interstitial fluid that does not directly return to blood vessels.
but first passes thru lymph nodes and then back to blood
Nutrients and oxygen diffuse from the blood into the interstitial fluid & then into the cells
Wastes and carbon dioxide move in the reverse direction
Composition of Blood
Blood is the body’s only fluid tissue
It is composed of liquid plasma and formed elements (Blood cells).
Formed elements include:
Erythrocytes, or red blood cells (RBCs)
Leukocytes, or white blood cells (WBCs)
Platelets
Hematocrit – the percentage of RBCs out of the total blood volume
Techniques of Blood Sampling
Venipuncture
sample taken from vein with
hypodermic needle & syringe
Why stick an vein?
less pressure
closer to the surface
Finger or heel stick
common technique for diabetics to monitor daily blood sugar
method used for infants
Physical Characteristics and Volume
Blood is a opaque fluid with a metallic taste
Color varies from red to dark red
Temperature is 38C, slightly higher than “normal” body temperature
Blood accounts for approximately 8% of body weight
Physical Characteristics
Thicker (more viscous) than water
Flows (Run)more slowly than water
pH 7.4 (7.35-7.45)
Blood volume
5 to 6 liters in average male
4 to 5 liters in average female
There is hormonal negative feedback systems witch maintain constant blood volume and osmotic pressure
التعليقات
Transportation
O2, CO2, metabolic wastes, nutrients, heat & hormones
Regulation
Regulate pH through buffers (As Phos +Bicar)
Regulate body temperature
High heat capacity and heat of vaporization for water
vasodilatation of surface vessels allow heat to give out to environment. Vasoconstriction of surface vessels reduces head emission to environment.
Regulate water content in cells by interactions with dissolved ions and proteins
Protection from disease & loss of blood
Components of Blood
Hematocrit
55% plasma
45% cells
99% RBCs
< 1% WBCs and platelets
Blood Plasma
0ver 90% water
7% plasma proteins
created in liver
limited to bloodstream
Albumin
maintain blood osmotic pressure
Globulins (immunoglobulins)
antibodies bind to foreignsubstances called antigens
form antigen-antibody complexes
Fibrinogen
for clotting
2% other substances
electrolytes, nutrients, hormones, gases, waste products
Functions of Blood :
Blood transports
Oxygen from the lungs and nutrients from the digestive tract
Metabolic wastes from cells to the lungs and kidneys for elimination
Hormones from endocrine glands to target organs
Regulation
Temperature by absorbing and distributing heat
PH in body tissues using buffer systems
Regulate water content in cells to gave adequate fluid volume in the circulatory system
Protection
Prevents from loss blood by:
Activating plasma proteins and platelets
Initiating the formation of clot when a vessel is broken
Prevents from infection by:
Synthesizing and utilizing antibodies
Activating complement proteins
Activating WBCs to defend the body against foreign invaders
Erythrocytes, leukocytes, and platelets
Only WBCs are complete cells
RBCs have no nuclei or organelles, and platelets are just cell fragments
Most blood cells survive in the bloodstream for only a few days
Most blood cells do not divide but are renewed by cells in bone marrow
Red blood cells ( erythrocytes )
White blood cells ( leukocytes )
granular leukocytes
neutrophils
eosinophils
basophils
agranular leukocytes
lymphocytes = T cells, B cells, and natural killer cells
monocytes
Platelets (special cell fragments)
Production of Leukocytes
There are 2 families of cytokines:
Interleukins (IL-1, IL-2)hematopoietic factors.
CSFs colony-stimulating factors for the WBCs stimulates granulocytes.
The important sources of cytokines are Macrophages and T cells.
Clinically many hematopoietic hormones are used to stimulate bone marrow
All leukocytes originate from Hemocytoblasts
Hemocytoblasts differentiate into:
Myeloid stem cells
Lymphoid stem cells
Myeloid stem cells become
Myeloblasts, Monoblasts, Erythroblasts
Lymphoid stem cells become lymphoblasts
Lymphoblasts develop into lymphocytes.
Myeloblasts develop into:Eosinophils, Neutrophils, and Basophils.
Monoblasts develop into monocytes
Agranulocytes Blood cells
Lymphocytes and monocytes
Lack visible cytoplasmic granules
Similar structurally but:
distinct functions.
and distinct cell types
Lymphocytes have spherical shape nuclei but the monocytes have kidney-shape nuclei.
Monocytes account 4–8% of leukocytes
Monocytes are the largest leukocytes
They have abundant pale-blue cytoplasm's
They have violet-staining nuclei.
The nuclei have U- or kidney-shaped.
Monocytes leave the circulation, enter tissue, and differentiate into macrophages
In infection take longer time to get to site of infection, but arrive in larger numbers
Become macrophages, once they leave the capillaries
Destroy microbes.
Clean up dead tissue following (after) an infection
Macrophages Function
Are highly mobile
Dynamically phagocytic
Activate lymphocytes to get bigger an immune response
Lymphocyte Functions
B cells
Destroy bacteria and their toxins
Turn into plasma cells that produces antibodies
T cells
Attack viruses, fungi, transplanted organs, cancer cells & some bacteria
Natural killer cells
Attack many different microbes & some tumor cells
Destroy foreign invaders by direct attack
Neutrophil Function
Fastest response of all WBC to bacteria
Direct actions against bacteria
Release lysozymes which destroy/digest bacteria
Release defensin proteins that act like antibiotics &
Poke holes in bacterial cell walls destroying them
Release strong oxidants (peroxide-like,strong
chemicals) that destroy bacteria
Eosinophil Function
Leave capillaries to enter tissue fluid
Release histaminase
slows down inflammation caused by basophils
Attack parasitic worms
Phagocytize antibody-antigen complexes
Basophil Function
Involved in inflammatory and allergy reactions
Leave capillaries enter connective tissue as mast cells
Release heparin & histamine
heighten the inflammatory response and account for hypersensitivity (allergic) reaction
Platelets are fragments of megakaryocytes with a blue-staining outer region and a lilac granular center
Their granules contain serotonin, Ca2+, enzymes, ADP, and platelet-derived growth factor (PDGF)
Platelets function in the clotting mechanism by forming a temporary plug that helps seal breaks in blood vessels
Platelets not involved in clotting are kept inactive by NO and prostaglandin I2
Proerythroblasts develop into early erythroblasts
The developmental pathway consists of three phases
Phase 1 – ribosome synthesis in early erythroblasts
Phase 2 – hemoglobin accumulation in late erythroblasts and normoblasts
Phase 3 – ejection of the nucleus from normoblasts and formation of reticulocytes
Reticulocytes then become mature erythrocytes
The number of erythrocytes remains constant and reflects a balance between RBC production and destruction
Too few red blood cells leads to tissue hypoxia
Too many red blood cells causes undesirable blood viscosity
Erythropoiesis is hormonally controlled and depends on adequate supplies of iron, amino acids, and B vitamins
Hormonal Control of Erythropoiesis
Erythropoietin (EPO) release by the kidneys is triggered by:
Hypoxia due to decreased RBCs
Decreased oxygen availability
Increased tissue demand for oxygen
worse erythropoiesis decreases the:
RBC count in circulating blood
Oxygen carrying ability of the blood
Erythrocytes (RBCs)
Erythrocytes are an example of the complementarity's of structure and function
Structural characteristics contribute to its gas transport function
Biconcave shape that has a vast surface area relative to volume
Discounting water content, erythrocytes are more than 97% hemoglobin
ATP is generated an aerobically, so the erythrocytes do not consume the oxygen they transport
Most blood cells types need to be continually replaced
die within hours, days or weeks
process of blood cells formation is hematopoiesis or hemopoiesis
In the embryo
occurs in yolk sac, liver, spleen, thymus, lymph nodes & red bone marrow
In adult
occurs only in red marrow of flat bones like sternum, ribs, skull & pelvis and proximal epiphysis of long bones
Pluripotent stem cells
0.1% of red marrow cells (can’t be distinguished from other cells)
replenish themselves as they differentiate into either myeloid or lymphoid stem cells
Myeloid stem cell line of development continues:
progenitor cells(colony-forming units) no longer can divide and are specialized to form specific cell types
example: CFU-E develops eventually into only red blood cells
next generation is blast cells
have recognizable histological characteristics
develop within several divisions into mature cell types
Lymphoid stem cell line of development
pre-B cells & prothymocytes finish their develop into B & T lymphocytes in the lymphatic tissue after leaving the red marrow
Available through recombinant DNA technology
recombinant erythropoietin (EPO) very effective in treating decreased RBC production because of end-stage kidney disease as well as treating anemias
other products given to stimulate WBC formation in cancer patients receiving chemotherapy which kills bone marrow
granulocyte-macrophage colony-stimulating factor
granulocyte colony stimulating factor
thrombopoietin helps prevent platelet depletion during chemotherapy
Globin protein consisting of 4 polypeptide chains
One heme pigment attached to each polypeptide chain
each heme contains an iron ion (Fe2+) that can combine reversibly with one oxygen molecule
Transport of O2, CO2 and Nitric Oxide
Each hemoglobin molecule can carry 4 oxygens molecules from lungs to tissue cells
Hemoglobin transports 23% of total CO2 waste from tissue cells to lungs for release
combines with amino acids in globin portion of Hb
Hemoglobin transports nitric oxide & super nitric oxide helping to regulate BP
RBCs live only 120 days
wear out from bending to fit through capillaries
no repair possible due to lack of organelles
Worn out cells removed by fixed/attached macrophages in spleen & liver
Breakdown products are recycled
Blood cells are replaced w/in 5-7 days after donation -uses up Fe3+ supplies
Blood bank makes you wait 8 weeks
Recycling of Hemoglobin Components
In macrophages of liver, spleen and/or red bone marrow
globin portion broken down into amino acids & recycled
heme portion split into iron (Fe3+) and biliverdin (green pigment)
Erythropoiesis: Production of RBCs
Requires Fe3+, vit B12, intrinsic factor, Erythropoetin, dietary protein
Proerythroblast starts to produce hemoglobin
Many steps later, nucleus is ejected & a reticulocyte is formed
Reticulocytes escape from bone marrow into the blood
In 1-2 days, they eject the remaining organelles to become a mature RBC
Feedback Control of RBC Production
Tissue hypoxia (cells not getting enough O2)
high altitude since air has less O2
Anemia: RBC production falls below RBC destruction
circulatory problems
Kidney response to hypoxia
release erythropoietin
speeds up development of proerythroblasts into reticulocytes
Normal Reticulocyte Count
Should be 0.5 to 1.5% of the circulating RBC’s
Low count indicate bone marrow problem
Leukemia
Nutritional deficiency.
or failure of red bone marrow to respond to erythropoietin stimulation
High count might indicate recent blood loss or successful iron therapy